Art as Therapy—Can Creative Expression Soothe Dementia Symptoms?
Quick Links
With a final stroke of the brush, Laura Baxter puts finishing touches on her painting, a piece of abstract art others deem a masterpiece. Baxter was diagnosed with Alzheimer’s disease at age 62. Now 77, she cannot remember how to sign her name without assistance. When she is done with her painting, she needs help finding her way to the bathroom down the hall and back to the art room, where several other people are creating their own works. “Are you Laura?” a woman asks, pointing to Baxter’s freshly signed painting. “It looks like you were sitting here.” Baxter smiles as she seems to recognize her own work, still glistening red with wet paint, and reclaims her spot at the table.
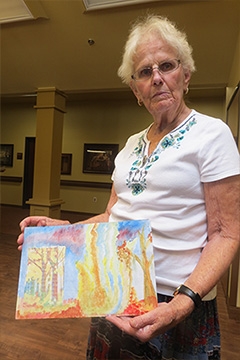
A woman with dementia displays her painting at Amber Grove Place in Chico, California. Caregivers at the assisted living community notice residents benefit in many ways from the creative arts. Image courtesy of Lorrie Badour, Amber Grove Place.
Scenes like this one at Amber Grove Place, an assisted living community for people with Alzheimer’s disease and other dementias in Chico, California, are emerging from a growing appreciation that the creative arts can help people with dementia in myriad ways. Art improves mood, reduces depression and anxiety, deepens connections with other people. In some cases, art even boosts cognition, claim some caregivers and clinicians who work with people engaged in this form of therapy. The evidence is largely qualitative and anecdotal, but some small placebo-controlled studies hint that the effects—which are inherently difficult to measure—may be real
Figuring out whether art therapy interventions benefit people with dementia is important. It’s also a tall order, said Anjan Chatterjee of the University of Pennsylvania in Philadelphia. With the dearth of pharmacological treatments for the burgeoning population of people with dementia, it is high time to explore artistic engagement for the relief of neuropsychiatric symptoms, Chatterjee told Alzforum. While there are drugs in the pipeline, none are imminent or expected to be a cure (see Alzforum Therapeutics database). “We are forced to think about what else can be done,” he said. Having recently published the book “The Aesthetic Brain: How We Evolved to Desire Beauty and Enjoy Art,” Chatterjee thinks the time is ripe for more research in the area. “There is an increased interest in art and the brain,” he said. “The zeitgeist seems ready for this.”
Excitement about art as therapy grew after the 2009 documentary “I Remember Better When I Paint.” Directed by Eric Ellena and Berna Huebner, whose mother painted prolifically before dying of Alzheimer’s disease, the film showcases initiatives around the world to engage people with dementia in art, whether by doing art projects inside assisted living facilities, by bringing people to museums, or by immersing them in other creative experiences. The movie draws upon the expertise of clinicians, caregivers, and art therapists, all of whom have witnessed the power of art in reaching those with dementia.

Berna Huebner drew upon her mother's experiences with art therapy for the documentary and the book "I Remember Better When I Paint." Courtesy of the Hilgos Foundation.
Huebner’s mother, Hilda Gorenstein, was a professional painter, but put her brushes aside after being diagnosed with AD in her 80s. She moved into a nursing home at age 90, and there she became anxious, apathetic, and aggressive—sometimes to the point of needing to be restrained. One day, when Huebner asked her mother if she’d like to paint, Gorenstein responded enthusiastically, “Yes, I remember better when I paint!” In response, Huebner invited students from the School of the Art Institute of Chicago to help her mother regain her skill and zest for the craft. After months of visits from one dedicated student, Jenny Graf Sheppard, Gorenstein gradually came out of her shell and started to paint. With the help of Sheppard and other students, Gorenstein produced around 300 paintings in the final years of her life. Doctors, caregivers, and family members noticed that the art sessions calmed Gorenstein, increased her focus, and made her receptive to communication.
“She was regaining the quality of life that she lost when she entered the nursing home,” recalled Sheppard in the film. According to Sheppard, the nursing home staff had subscribed to the idea that the “lights were off” for Gorenstein, and that she was no longer capable of engaging meaningfully. Huebner described her mother’s resurgence as a breakthrough, and hopes to share the same experience with others. She founded the Hilgos Foundation, which awards scholarships to students at the School of the Art Institute of Chicago to involve people with dementia in the arts.

Buoyed by dedicated students, artist Hilda Gorenstein painted prolifically in the final years of her life before succumbing to Alzheimer’s. From "I Remember Better When I Paint,” courtesy of the Hilgos Foundation.
While Gorenstein’s comeback is but one anecdotal account, other caregivers and researchers claim to have witnessed similar transformations. Judy Holstein, who is featured in the film and previously directed art programs at the Council for the Jewish Elderly in Chicago, told Alzforum that art engagement leads to closer connection with others, better attention, and greater mental and physical well-being. People tend to focus deeply during creative activities, become more present, and forget about aches, pains, and other things that would otherwise cause agitation, Holstein said. She recalled one instance when a woman who used a walker left it behind to participate in a drama session. Art can serve as a healthy outlet for people to express their fears, she said. “When you engage in art, you know your sense of well-being and inner and outer health is improved, not just during it, but afterwards,” she said.
Others extol the benefits of bringing people to art, rather than bringing art to people. Sean Caulfield is the co-founder and creative director of ARTZ: Artists for Alzheimer’s. This Boston-based nonprofit, also featured in Huebner’s documentary, creates guided, interactive programs at museums, parks, theaters, and other stimulating environments where people with dementia and their caregivers can engage. ARTZ focuses on getting people with dementia out into the community. Last year its museum program, “Meet Me at the Museum,” drew 800 people from 48 different care facilities, Caulfield said. “Consciousness is being raised about the idea that ‘getting out’ is therapy for all of us, and when people are deprived of that, their condition can worsen,” he said.
Like Holstein, Caulfield speaks of improvements in mood and communication. By acknowledging nonverbal forms of communication among the participants, such as a smile or thoughtful glance at a painting, program leaders sometimes find that people who had stopped speaking will suddenly pipe up. “Once the person’s anxiety about speaking is removed, and they feel accepted, that person will then speak. It just comes right out,” Caulfield said. While these momentary breakthroughs may not happen directly because of the art, Caulfield said it works as a catalyst. “That’s what makes art the great equalizer. By removing some of the physical, environmental, and social barriers, we’re left with the person.”
Where is the Proof?
While firsthand accounts of the transformative power of art in dementia abound, controlled trials do not. Chatterjee, who believes that engagement in the arts benefits people with dementia, readily concedes that solid research is lacking. “People have intuition but what is the evidence?” he asked. Chatterjee and colleagues recently reviewed the literature (see Chancellor et al., 2014), uncovering a dozen case studies and four randomized controlled trials. Together they point to neuropsychiatric benefits of art engagement for people with dementia, but most were methodologically weak, Chatterjee said. “The problems with the studies are typically that they are anecdotal, or lack proper control groups. Also, they haven’t looked at basic questions of how many sessions there should be, or whether the effects generalize beyond the sessions, ” he said.
One study led by Diane Waller of the University of London, U.K., compared cognitive and psychological changes in people with dementia who had weekly art therapy sessions to those in people who took up other recreational activities for 40 weeks (see Rusted et al., 2006). The people in the art group became mentally sharper, calmer, and more social compared to those in the recreational group. After the study, participants in the art therapy group became more depressed for a while. Conclusions were hard to draw, however, because only 21 of the 45 people enrolled in the trial completed it, and had been diagnosed with several different kinds of dementia to begin with.
Another study, led by Toru Mase at the National Center for Geriatrics and Gerontology in Obu, Aichi, Japan, enrolled 39 people with mild Alzheimer’s disease in a 12-week trial that compared the cognitive and psychological effects of weekly art therapy to those of sessions where participants tried to solve math problems. Quality of life reportedly improved modestly for those in the art therapy sessions (see Hattori et al., 2011).
Chatterjee said future studies should parse out which kinds of art therapy most benefit people with dementia. The ideal study would start with people in similar stages of the same disease, intervene several times per week over the course of months, and incorporate appropriate control therapies based on social activity. He also suggested tracking whether benefits to patients persist beyond the art sessions, and whether the mental health of caregivers improves. Such studies would be time-intensive and costly, he said. “Funding would have to come from the government, but there’s more of a push towards biologically oriented interventions,” he said.
Does Art Defy Dementia?
Many reports on art’s effects on people with dementia are case studies. Luis Fornazzari of the University of Toronto has published a handful over the past decade, documenting that artistic or musical ability is relatively preserved in people with dementia (see Fornazzari, 2005; Fornazzari et al., 2006). Most recently he published a collection of sketches the sculptor Mary Hecht made as she struggled with severe vascular dementia in the last years of her life (see Fornazzari et al., 2013). While Hecht scored low on cognitive tests such as the mini-mental state exam and, oddly enough, the clock drawing test, she produced detailed drawings of other things from memory, such as one of a reclining Buddha, and one of a famous cellist she had seen years before. “She proved the point that art, regardless of progressive dementia, is more resistant to neurodegenerative pathologies,” Fornazzari claimed. He also noted that Hecht came alive whenever art came up in conversation. “She couldn’t recall my name or who I was, but everything in the realm of art was there and fresh and ready to be discovered,” he told Alzforum. “The art was preserved, but the mundane, day-to-day things were impaired.” Fornazzari claims to have witnessed a similar preservation with other artists and musicians with Alzheimer’s disease.
In some cases, particularly in people with frontotemporal dementia (FTD), new artistic abilities emerge as the disease progresses. Bruce Miller of the University of California, San Francisco, recalled a businessman who had never painted before entering a period of “artistic brilliance” (see Miller et al., 1996). Miller observed similar episodes in other FTD patients, including, most famously, the scientist Anne Adams, who painted renderings of musical compositions while sliding into progressive aphasia (Seeley et al., 2008; see also New Scientist story). Although most patients with dementia never become renowned artists, the observation that their artistic expression remains intact while other faculties deteriorate could indicate that art poses a unique avenue of expression for those with dementia, said Miller. “These observations have taught me that despite the degenerative process, there’s a human being inside. There are things that give dementia patients great pleasure, and they still have potential,” he said.
Other clinicians make similar observations treating a disease that, like Alzheimer’s, devastates some parts of the brain and leaves others relatively spared. “Although verbal memory is almost always affected early, the disease is different in everyone,” said Brad Hyman of Massachusetts General Hospital. “I frequently ask our families to try nonverbal communication and skills, and in some cases this can be art. One of my patients recently won a local art contest despite struggling with our ‘standardized' tests. Others respond well to music. Not every patient benefits. Even so, I concur with the idea that even in advanced dementia there is a person alive inside, and am committed to finding ways to help get them out,” he said.
In 2007, Miller compared art by people with FTD or AD to that made by healthy controls using raters blinded to each person’s diagnosis. People with FTD tended to produce disorganized yet vivid art, whereas people with AD tended to paint with muted colors and produce slightly distorted images (see Rankin et al., 2007). Miller thinks these artistic differences reflect the parts of the brain respectively ravaged by the each disease. When the frontal lobes degenerate, as in FTD, executive function and language suffer but visual processing may get a boost. In contrast, because Alzheimer’s progresses to the back of the brain where visuospatial processing occurs, this disease could lead to less vibrant or distorted drawing, Miller said. Overall, he believes that when certain parts of the brain degenerate, others become more active. “There’s this constant back and forth of one circuit turning off and the other turning on,” he said. This would explain why a subset of people with FTD may suddenly experience intense visual perception and hence be drawn to producing art, he said.
Even so, Miller doubts that creating or enjoying art can improve cognitive function or slow neurodegeneration in dementia. “I don’t think it changes the course of the disease, but it’s symptomatic therapy,” he said. Not all patients enjoy producing art, he added, and the type of creative activity to which people gravitate—including dancing or music—varies from person to person.
Miller champions the biological focus at the nation’s funding agencies, because finding cures for dementia should be the ultimate goal, he said. In the meantime, other interventions are sorely needed. “People live a long time with these diseases, so these other therapies are also important and their study should be funded,” he said.
Other leading Alzheimer’s researchers agree that rigorous data on art therapy may be hard to get. “A key challenge with dietary or lifestyle interventions is reducing things to a prescription. We can now do that with physical exercise (three 30-minute sessions per week of weight training or brisk walking), but factors such as mental and social engagement cannot yet be reduced to a randomized, controlled trial. As a result we do not have an evidence-based regimen we can prescribe. The same is true of art therapy,” said Sam Gandy of Mount Sinai School of Medicine in New York. “Still, art may improve quality of life for patients and caregivers, even if temporarily. Anything that brings respite and joy into their lives is worth a shot while we are chasing down the science.”—Jessica Shugart
References
Paper Citations
- Chancellor B, Duncan A, Chatterjee A. Art Therapy for Alzheimer's Disease and Other Dementias. J Alzheimers Dis. 2013 Oct 10; PubMed.
- Hattori H, Hattori C, Hokao C, Mizushima K, Mase T. Controlled study on the cognitive and psychological effect of coloring and drawing in mild Alzheimer's disease patients. Geriatr Gerontol Int. 2011 Oct;11(4):431-7. PubMed.
- Fornazzari LR. Preserved painting creativity in an artist with Alzheimer's disease. Eur J Neurol. 2005 Jun;12(6):419-24. PubMed.
- Fornazzari L, Castle T, Nadkarni S, Ambrose M, Miranda D, Apanasiewicz N, Phillips F. Preservation of episodic musical memory in a pianist with Alzheimer disease. Neurology. 2006 Feb 28;66(4):610-1. PubMed.
- Fornazzari L, Ringer T, Ringer L, Fischer CE. Preserved drawing in a sculptor with dementia. Can J Neurol Sci. 2013 Sep;40(5):736-7. PubMed.
- Miller BL, Ponton M, Benson DF, Cummings JL, Mena I. Enhanced artistic creativity with temporal lobe degeneration. Lancet. 1996 Dec 21-28;348(9043):1744-5. PubMed.
- Seeley WW, Matthews BR, Crawford RK, Gorno-Tempini ML, Foti D, Mackenzie IR, Miller BL. Unravelling Boléro: progressive aphasia, transmodal creativity and the right posterior neocortex. Brain. 2008 Jan;131(Pt 1):39-49. Epub 2007 Dec 5 PubMed.
- Rankin KP, Liu AA, Howard S, Slama H, Hou CE, Shuster K, Miller BL. A case-controlled study of altered visual art production in Alzheimer's and FTLD. Cogn Behav Neurol. 2007 Mar;20(1):48-61. PubMed.
Other Citations
External Citations
Further Reading
Papers
- Gretton C, ffytche DH. Art and the brain: a view from dementia. Int J Geriatr Psychiatry. 2013 Aug 8; PubMed.
Annotate
To make an annotation you must Login or Register.

Comments
I am an art and sandplay therapist. I know that the potential of art for people who, for whatever reason, have lost the ability to express themselves clearly has not even been dreamed of. I have had success through art and sandplay, where all other methods have failed.
Make a Comment
To make a comment you must login or register.