Miami: Amyloid in the Aging Brain—What Does It Mean?
Quick Links
At the 5th annual Human Amyloid Imaging meeting, held 14-15 January 2011 in Miami, Florida, the bulk of the talks and posters reflected scientists’ grappling with how amyloid deposition in the brain behaves over time and what it does to the brain’s ability to function. The field appears to agree that it’s bad for the brain; beyond that, exploratory results and new ideas dominated the discussion.
Annie Cohen of the University of Pittsburgh Medical School, Pennsylvania, started things off with her new data on the fundamental question of how the amount of Aβ people harbor in their brains changes over time. The general idea these days is that brain amyloid begins to rise with age, in people’s fifties and sixties, about a decade earlier in people with ApoE4 than those without (and earlier still in people with autosomal-dominant mutations). This starts some 15 years prior to a clinical diagnosis of dementia; after that diagnosis, amyloid levels stay largely the same during the person’s last decade or so of life with mild to moderate, and then severe dementia. Biomarker staging diagrams shown at conferences these days (e.g., Jack et al., 2009; ARF Webinar) depict brain amyloid levels swinging up with age in an S-shaped curve, though in truth, researchers readily acknowledge they don’t know for sure yet what shape that curve takes, and whether it levels off completely. Some studies have suggested that the increases over time are more straight than S-shaped; others that brain Aβ keeps rising through the course of diagnosed AD dementia. “Whether amyloid deposition goes up linearly or in a sigmoid fashion is very important later for the use of biomarkers in therapeutic trials,” said Keith Johnson of the Massachusetts General Hospital. A definitive answer will come from more data on more people from more time points in longitudinal studies; meanwhile, here is the latest cut from Miami.
Cohen reported that in her group of 55 cognitively normal controls, 27 people with MCI, and 16 with AD, PIB retention over the course of three years did increase in more than half of those with AD. In the control and MCI cases, brain amyloid progressively rose in those who had started out PIB positive, and in some who had started out PIB negative, though many of the latter at this point remain below a set threshold of "PIB positivity." “We think amyloid accumulates in a linear manner over time,” Cohen said. In a study that primarily probed technical aspects of this question by comparing different imaging processing methods in ADNI participants, Susan Landau at University of California, Berkeley, also saw a small increase in amyloid load over time in people with AD.
In contrast, Jaana Koivunen of the PET Centre in the Finnish city of Turku reported data more in synch with the idea that PIB deposition is largely complete by the time of an AD dementia diagnosis. Koivunen follows 29 people in their seventies with MCI using PIB-PET, MRI, and neuropsychometry. She reported that 17 volunteers who met criteria for probable AD two years after baseline had started out with higher amyloid deposition at baseline than did volunteers who did not progress clinically, but these 17 added no further amyloid since baseline. In contrast, the 12 who clinically progressed little in those two years were still adding more amyloid, raising the question of whether they might reach the AD diagnosis in the future. Hippocampal atrophy increased in both groups, similar to earlier one-year follow-up data from the Mayo Clinic in Rochester, Minnesota (Jack et al., 2009). On a poster, Rik Ossenkoppele at the VU Medical Center in Amsterdam, The Netherlands, similarly reported that the curve rose in the MCI group and flattened off in AD.
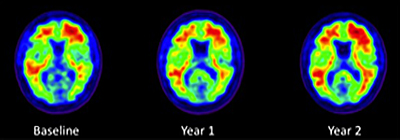
Three PIB-PET scans taken two years apart in an ADNI normal control show modest expansion of brain amyloid over the course of two years. Image credit: Susan M. Landau, UC Berkeley
In discussion, Michael Pontecorvo from Avid Radiopharmaceuticals noted that even his company’s larger dataset of many hundreds of patients imaged prospectively with florbetapir does not to date support the drawing of a more precise staging curve, as no one has yet figured out how to analyze all the factors that affect amyloid deposition over time. One problem, said PIB co-developer Chet Mathis of the University of Pittsburgh Medical School is that group averages obscure change in individual people. In a given person, scientists do see a large jump in one year, and a leveling off the next. “We will get at the shape of the curve once we have enough data on enough subjects for statistically sound modeling, but at this point we lose the dynamic view because we present group averages,” Mathis said. Scientists need more data to get a handle on a related issue, as well: namely the time course of when different brain areas, especially those affected later, deposit AD. These areas keep changing deeper into the course of disease, but no comprehensive view of their sequence in time is yet in sight.
Diagnosed AD aside, the earliest phase of amyloid deposition increasingly commands researchers’ attention. Does having “a head full of amyloid” mean a non-demented person is heading toward AD? What factors play into this question? This is where multimodal studies come in.
First, an attempt to account for cognitive reserve. Numerous studies have pinned a degree of protection from AD on education and intelligence. Dorene Rentz of Massachusetts General Hospital, Boston, shared the latest data on 84 non-demented research volunteers in their seventies who had a PIB-PET scan at baseline. At that point, they scored a perfect 0 or a 0.5, indicating very mild/prodromal symptoms on the Clinical Dementia Rating (CDR) scale and then underwent subsequent neuropsychological testing over some 18 months to date of follow-up. In Miami, Rentz showed results of multivariate modeling with those data, which sought to unpack the effects of amyloid and cognitive reserve.
Having amyloid in the precuneus/posterior cingulate areas of the brain at baseline predicted that the person would subsequently decline in AD-relevant cognitive domains. Overall, people with high cognitive reserve withstood brain amyloid better than people with low cognitive reserve. However, within those groups, Rentz spotted some differences. People positive for brain amyloid who had high cognitive reserve declined mostly in memory tasks, particularly immediate and delayed recall. People positive for brain amyloid with low cognitive reserve tended to fall off on a broader range of tests. This included memory for cued and delayed recall such as is used in the Dubois criteria for prodromal AD (e.g., the free and cued selective reminding test, FCSRT), and visuospatial perception. Regardless of their cognitive reserve, all volunteers who had low brain amyloid improved with repeated testing, whereas volunteers with high amyloid showed no such practice effect. At the same time, regardless of amyloid, highly educated people were more cognitively stable than less educated fellow volunteers.
In short, the take-home message at this early point of this prospective study is that mounting levels of amyloid do portend cognitive decline, but high education shields against that. This means that competing factors at work in a given person complicate the relationship between amyloid and cognitive decline. And reporting from a longstanding longitudinal study of highly educated, otherwise healthy people that is now incorporating florbetapir PET scans, Karen Rodrigue from the University of Texas at Dallas correlated increasing cortical amyloid with a slowdown in processing speed.
Following amyloid deposition in longitudinal cohorts is necessary for many reasons. One is that cognitive reserve is one likely reason for the great variability researchers see in how well people tolerate brain amyloid. It could explain the nagging puzzle of a group of people in aging studies that Susan Resnick of the National Institute on Aging in Bethesda, Maryland, brought up: namely those who die without a known history of cognitive decline but upon autopsy prove to have had AD per the disease’s pathological definition. This finding lingers as a criticism of the amyloid hypothesis. Since it is a postmortem finding, it’s unclear if the person’s amyloid developed many years or shortly before death. Had the person lived, how long until dementia set in? A year? A decade? In discussion, other scientists cautioned that such studies sometimes apply a low pathological threshold to declare AD and that the cognitive instruments in some older longitudinal studies fail to pick up the subtle episodic memory problems of preclinical AD. More current studies looking at amyloid and other outcomes simultaneously do indicate that this pathology has consequences for cognition and even activities of daily living. For example, a poster presented at HAI by Gad Marshall of Massachusetts General Hospital found that among a group of 55 subjects with MCI or normal cognition from ADNI and an ancillary study, those who had the most brain amyloid also were the most impaired in high-level skills used in everyday tasks (such as shopping, handling finances), even after controlling for the impact of memory impairment. These results were driven by the MCI subjects.
In between amyloid deposition and the ultimate outcomes of cognition and daily function lies the big territory of what might be the neural substrates for any damage downstream of amyloid. This question has an existing literature of toxicity pathways from cell-based and animal model studies, but bringing human imaging to bear on it is largely unexplored space. Early forays into the new world of combined amyloid, FDG-PET, and fMRI connectivity imaging were on display in Miami. See Part 3 of this series.—Gabrielle Strobel.
This is Part 2 of a seven-part series. See also Part 1, Part 3, Part 4, Part 5, Part 6, Part 7. View a PDF of the entire series.
References
Webinar Citations
News Citations
- Miami: Multimodal Imaging, New Way to Test Amyloid Hypothesis
- Miami: Women Rock at Human Amyloid Imaging Meeting
- Miami: Astrocytes, Antidepressants, Microbleeds, and More
- Miami: Updates on J-ADNI, 18F Tracers, Biopsies
- Miami: Is Human Amyloid Imaging Ready for Clinical Trials?
- Miami: HAI Amyloid Imaging Conference Abstracts
Paper Citations
- Jack CR, Knopman DS, Jagust WJ, Shaw LM, Aisen PS, Weiner MW, Petersen RC, Trojanowski JQ. Hypothetical model of dynamic biomarkers of the Alzheimer's pathological cascade. Lancet Neurol. 2010 Jan;9(1):119-28. PubMed.
- Jack CR, Lowe VJ, Weigand SD, Wiste HJ, Senjem ML, Knopman DS, Shiung MM, Gunter JL, Boeve BF, Petersen RC. Serial PIB and MRI in normal, mild cognitive impairment and Alzheimer's disease: implications for sequence of pathological events in Alzheimer's disease. Brain. 2009 May 1;132(Pt. 5):1355-65.
Other Citations
Further Reading
Annotate
To make an annotation you must Login or Register.

Comments
No Available Comments
Make a Comment
To make a comment you must login or register.